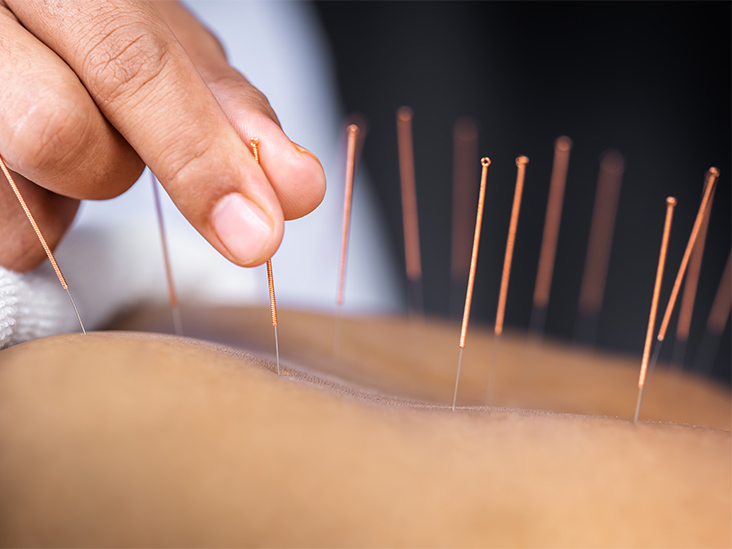
Vielight Neuro 3 is the world’s best brain photobiomodulation device. Our patented transcranial-intranasal technology offers an unparalleled advantage for reaching both the ventral and cortical layers of the brain. The Vielight Neuro is available in three models: the Alpha, the Gamma, and the Duo. It is a next-generation brain stimulation device based on the science of photobiomodulation (PBM). It delivers an 810 nm near infrared (NIR) energy via four transcranial LED modules and a nasal applicator. The headset’s transcranial LED modules target the hubs of the brain’s default mode network (DMN), which often represent the overall health of the brain.
How does photobiomodulation affect inflammation, pain, and tissue healing?
Reative oxygen species play a central role in the progression of inflammation. During inflammatory conditions, ROS production causes an increase in the migration of inflammatory cells to the damaged tissue. Furthermore, polymorphonuclear neutrophils (PMNs) increase ROS production at the location of inflammation. In turn, this causes dysfunction within endothelial cells and additional tissue injury.
The migration of inflammatory cells results in more injury in inflamed tissue, as well as pain, delaying the healing process (Mittal et al., 2014). PBM (with light using wavelengths greater than 500 nm) increases the production of ROS in normal cells (Chen et al.). Thus, it reduces markers of oxidative stress in stressed and damaged cells (de Freitas & Hamblin, 2016), demonstrating that photobiomodulation promotes faster healing.
Furthermore, PBM can suppress inflammation by reduction in PGE2- levels and inhibition of cyclooxygenase-2 (COX-2) in cells (Bjordal et al., 2003). Cyclooxygenase-2 is an enzyme responsible for inflammation and pain. Therefore, the appropriate dose of PBM directed to the injured tissue could positively control pain, reduce inflammation, and expedite healing.
Although the pain control mechanisms of PBM are not yet clearly understood, several theories have been proposed. The regulation of pain (Melzack & Wall, 1965), modulation of inflammation, upregulation of β-endorphin production (Laakso et al., 1994), direct inhibition of neural activity (Snyder-Mackler & Bork, 1988), and acceleration of healing are all mechanisms by which PBM is thought to control pain.